Urinary incontinence, the involuntary leakage of urine, is a common condition affecting a significant portion of the population. It can impact individuals of all ages, but is more prevalent among older adults and women. The condition not only affects physical health but also emotional and social well-being.
Types of Urinary Incontinence
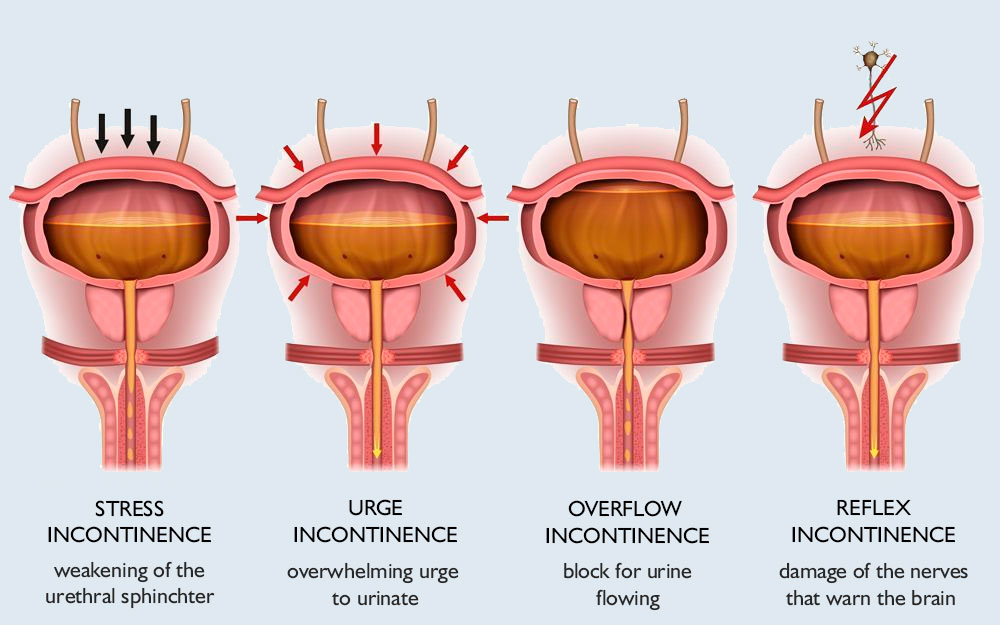
Understanding the type of incontinence is crucial for effective treatment:
- Stress Incontinence: Caused by weakened pelvic floor muscles. Activities that increase abdominal pressure, like coughing or exercising, can lead to urine leakage.
- Urge Incontinence: Also known as overactive bladder, this involves a sudden, intense urge to urinate, followed by involuntary leakage.
- Mixed Incontinence: A combination of stress and urge incontinence.
- Functional Incontinence: Due to physical or cognitive impairments that make it hard to reach the toilet in time.
- Overflow Incontinence: Occurs when the bladder doesn’t empty completely, leading to frequent or constant dribbling.
Causes and Risk Factors
Several factors contribute to urinary incontinence:
- Age: Muscle weakening with age can lead to incontinence.
- Gender: Women are more prone due to childbirth and menopause.
- Obesity: Excess weight increases pressure on the bladder.
- Smoking: Can lead to cough-induced stress incontinence.
- Chronic Diseases: Conditions like diabetes and neurological disorders can affect bladder control.
Diagnosing Urinary Incontinence

Diagnosing urinary incontinence typically involves a comprehensive assessment starting with a detailed medical history to understand the patient’s symptoms, lifestyle habits, and any relevant past medical issues. This is followed by a physical examination, where a healthcare provider checks for any physical signs that might be affecting the urinary tract. An important step in the evaluation is a urinalysis, which helps to rule out infections or other underlying conditions that could be contributing to incontinence. Patients are often asked to keep a bladder diary, where they record their fluid intake, the times they urinate, and any instances of leakage. This diary provides valuable insights into the patient’s urinary patterns and helps in planning treatment. Additional diagnostic tests, such as urodynamic testing, may also be conducted. These tests assess bladder function and help pinpoint the specific type or cause of urinary incontinence, guiding the development of an effective treatment plan.
Treatment Strategies
Lifestyle and Behavioral Interventions
- Pelvic Floor Exercises (Kegels): Strengthening the muscles that control urination.
- Bladder Training: Gradually increasing the intervals between urinating.
- Dietary Adjustments: Avoiding irritants like caffeine and alcohol.
- Weight Management: Reducing obesity-related pressure on the bladder.
Medical Treatments
- Medications: Drugs to relax the bladder or tighten muscles at the bladder neck.
- Topical Estrogen: For postmenopausal women to rejuvenate deteriorating tissues.
- Nerve Stimulation: Electrical stimulation procedures such as EMSELLA to control bladder and sphincter muscles.
Surgical Options
- Sling Procedures: Supporting the bladder neck or urethra.
- Bladder Neck Suspension: Providing support to the urethra and bladder neck.
- Artificial Urinary Sphincter: Implanting a device to control urine flow.
Coping and Support

Living with urinary incontinence often demands a great deal of emotional resilience. To help address the emotional and psychological impacts that often accompany this condition, counseling can be an invaluable resource. It provides a space to discuss feelings and develop coping strategies. Additionally, joining support groups can be highly beneficial. In these groups, individuals share their experiences and strategies, offering comfort and practical advice to others facing similar challenges. Alongside these emotional support mechanisms, practical management of incontinence involves the use of protective products. Pads or special underwear designed for incontinence can significantly help in managing leaks, offering both physical comfort and peace of mind. These combined approaches – emotional support through counseling and support groups, and practical management with protective products – play a crucial role in helping individuals navigate the challenges of living with urinary incontinence.
The Role of Healthcare Providers
Regular consultations with healthcare professionals are vital for:
- Personalized Treatment Plans: Tailored to individual needs and types of incontinence.
- Monitoring Progress: Adjusting treatments based on response.
- Addressing Complications: Preventing and treating urinary tract infections or skin irritation.
A Path to Improvement
Urinary incontinence, while challenging, can often be managed effectively. The combination of lifestyle changes, medical interventions, and support can lead to significant improvements in quality of life. Regular medical consultations are crucial for ongoing management and adapting treatment plans as needed.
Remember, the experience of urinary incontinence is unique to each individual, and what proves effective for one person may not yield the same results for another. It’s a journey of discovering the right mix of treatments, lifestyle changes, and support systems. If you’re exploring various treatment options and feel that EMSELLA, a non-invasive therapy, might be suitable for you, consider contacting Chandra Wellness for a consultation. With persistence and a tailored approach, many people find that their symptoms improve significantly over time.